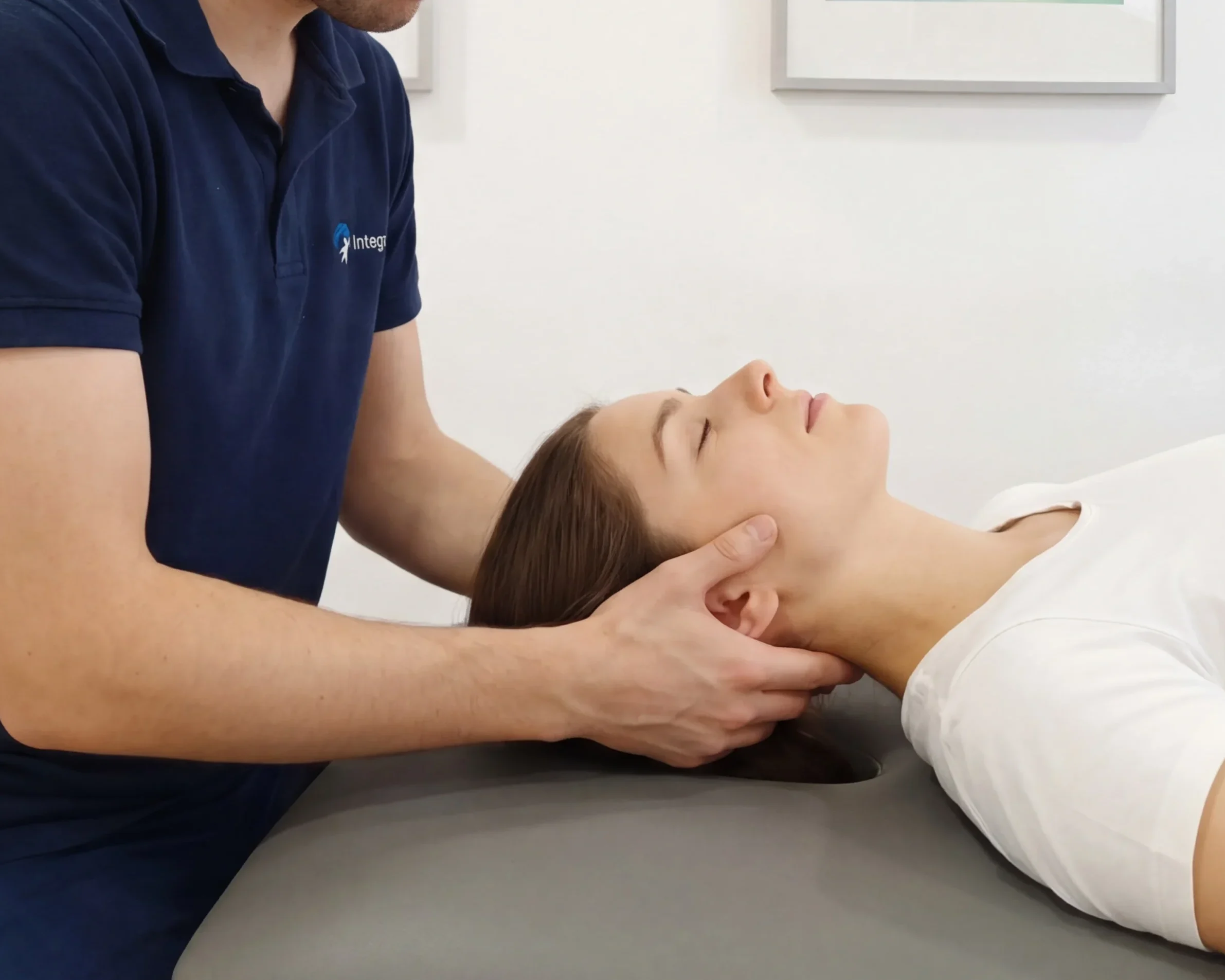
Neck pain, also referred to as cervicalgia, is pain located in the neck region and is part of the broader category of spinal pain, potentially coexisting with back or lumbar complaints. Neck pain is one of the most common musculoskeletal complaints in the adult population, with a significant impact on daily functionality, professional performance, and overall well-being.
According to data widely cited by the World Health Organisation, a significant proportion of the population will experience back pain during their lifetime. In many cases, cervical episodes are acute and resolve favourably over days or weeks. Nevertheless, the intensity of the symptoms and the associated functional limitation justify a careful clinical evaluation and an Osteopathic approach tailored to the individual context.
Currently, neck pain is understood as a complex and multifactorial phenomenon, influenced by physical, neurological, emotional, social, and contextual components, a framework that underpins contemporary person-centred intervention models, including approaches such as Osteopathy.
What is understood by neck pain
Neck pain can appear suddenly or progressively and have different characteristics, such as a feeling of heaviness, stiffness, burning or stabbing. It can be localised or radiate to the shoulders, interscapular region or upper limbs, manifest intermittently or persistently and be associated with limited movement, headaches or sensory changes.
From a clinical perspective, a significant portion of neck pain is classified as non-specific, meaning there is no single, clearly identifiable structural cause on imaging. In cases of neck pain, several mechanisms are often involved simultaneously, including changes in joint mobility, increased muscle tone, alterations in movement control, and nervous system sensitisation, where stimuli that are normally neutral are perceived as uncomfortable.
This understanding moves away from an exclusively mechanical view of neck pain and reinforces the importance of integrative approaches, such as Osteopathy, which consider multiple dimensions of the clinical experience.
Factors such as high stress levels, irregular sleep patterns, fear of movement, prolonged posture in front of screens, or previous negative experiences associated with pain can influence the progression of cervicalgia. These aspects are now recognised as an integral part of clinical assessment in Osteopathy.
Common types of neck pain and associated mechanisms
Neck pain can be related to different structures and systems, and it is common for several mechanisms to coexist:
- Cervical disc changesThe cervical intervertebral discs play a central role in impact absorption and neck mobility. In cases of disc degeneration or protrusion, local inflammatory phenomena and chemical sensitisation can occur, contributing to neck pain and sometimes radiating pain down the arm.
- Cervical root painCharacterised by pain radiating to the upper limb, which may be associated with tingling, numbness, or loss of strength. It generally results from a combination of mechanical compression and inflammatory irritation of the nerve roots. It is important to note that imaging findings do not always correspond to the intensity of the symptoms.
- Cervical facet arthropathyThe facet joints contribute to the fine control of cervical spine movement. With disc aging or postural overload, these joints can develop degenerative changes, manifesting as local pain or pain referred to the shoulders and the interscapular region.
- Myofascial painMuscles and fasciae, such as the scalenes, levator scapulae, trapezius, suboccipitals, and deep cervical musculature, play a significant role in stability and proprioception. Spasm, overload, or altered activation patterns can generate local pain and referred tension points.
- Cervicogenic headachesChanges in the mobility of the upper cervical segments or increased suboccipital muscle tone can contribute to cervicogenic headaches.
- The relationship between visceral dysfunction and neck painVisceral stimuli can influence the cervical region via neurological pathways and fascial continuities, causing increased muscle tone or referred pain in segments with the same innervation.
The evolution of neck pain varies widely among individuals. Some episodes resolve spontaneously, while others tend to become recurrent, particularly when mechanical, emotional, and contextual factors coexist.
The relationship between visceral dysfunction and neck pain
Internal organs have physiological mobility necessary for their function. Restrictions in this mobility can influence the cervical region through fascial connections and neurological pathways. The viscero-somatic reflex describes how stimuli from internal structures can originate an increase in muscle tone or pain in areas with the same segmental innervation, with this interaction being considered in Osteopathic assessment, especially in persistent cases.
Beyond neurosegmental mechanisms, there is also a mechanical continuity between the pleura, cervical spine and superior mediastinum through fascial thickenings often described as vertebro-pleural ligaments. These structures connect the pleural apex to the lower cervical vertebral bodies and the prevertebral fascia, contributing to the stability of the pleural dome during respiration.
In contexts where pleural mobility is restricted or there's increased tension in the upper thoracic fascia, as can happen with altered breathing patterns, inflammatory processes, or mechanical overload, tension can be transmitted to the lower cervical segments. This connection should not be understood as a sole, direct cause of neck pain, but rather as a possible additional mechanical contributor that, along with viscerosomatic convergence and adaptation of respiratory motor control, can play a part in maintaining persistent neck pain conditions.
The osteopathic view of neck pain
Osteopathy is a manual clinical practice based on the assessment of the relationships between the musculoskeletal system, fascial structures, the nervous system, and internal organs, recognising the functional interdependence between these components.
In neck pain, the process begins with a detailed assessment, which includes:
- Complete medical history (onset of symptoms, aggravating or relieving factors, functional impact)
- Postural observation and movement analysis
- Palpation of tissues, joints and musculature
- Alarm signal tracking, with forwarding when indicated
From this assessment, clinical hypotheses are formulated, guiding the approach, always adapted to the specific needs of each person.
The cervical region, due to its high mobility and integration with the visual, vestibular, and respiratory systems, is particularly sensitive to factors such as sustained posture, stress, and altered breathing patterns. It is common to observe increased stiffness in this area in contexts of prolonged tension.
How osteopathy works on neck pain
A Osteopathic approach For neck pain, selected manual techniques are used based on clinical findings, integrated into an individualized plan that considers the person's overall functioning.
Depending on the clinical context, strategies such as:
- Cervical and thoracic spinal mobilization
- Soft tissue techniques targeting superficial and deep musculature
- Fascial normalization of cervico-scapular chains
- Muscle energy techniques
- Gentle neurodynamic approaches
- Low-amplitude joint techniques, adapted to individual tolerance
- Visceral integration in specific contexts
- Breathing exercises, enhancing diaphragm function and autonomic nervous system regulation
These interventions are part of a broader plan which may include pain education, guidance for progressive physical activity, simple mobility and motor control exercises, as well as respiratory and self-regulation strategies.
The clinical objective is to support mobility improvement, modulate the nervous system's response and promote more efficient movement patterns, while simultaneously encouraging the individual's active participation in the therapeutic process.
Some common myths about neck pain
Ideas persist that prolonged rest is necessary or that changes observed in imaging scans always explain the pain. In clinical practice, gradual mobilisation adapted to individual tolerance tends to be associated with better outcomes, and functional assessment is central to understanding non-specific neck pain.
The clarification of these aspects is part of the health education process, contributing to more realistic expectations throughout the follow-up.
When to consider assessment in Osteopathy
Neck pain does not always resolve spontaneously, especially when episodes recur or when functional limitation interferes with daily life.
Is it worth seeking an Osteopathy referral when there is:
- Persistent neck pain for more than two weeks
- Recurring episodes that return frequently
- Limited range of motion — difficulty turning or tilting the head
- Pain radiating to the shoulders, interscapular region, or upper limbs
- Tension-type headaches associated with neck tension
- Pain that is aggravated by prolonged posture, stress, or fatigue
- Feeling of stiffness or heaviness in the neck upon waking
Osteopathic assessment can incorporate cases of acute, subacute, or persistent cervical pain, working in conjunction with Physiotherapy, therapeutic exercise, or other clinical areas, always in a coordinated manner and adapted to individual progression.
Understanding Osteopathy in Neck Pain from an Integrative Perspective
A Osteopathy It fits current models of care for neck pain by combining rigorous clinical assessment, manual intervention, and health education. Embedded in a person-centred practice, it constitutes a valid approach to supporting the management of this common condition, respecting the complexity of its mechanisms and the uniqueness of each clinical journey.
In an Integrative Osteopathy consultation, neck pain is assessed by considering the interactions between the musculoskeletal, visceral, and cranial systems, as well as factors such as breathing patterns, sleep quality, stress levels, and movement habits. This holistic view allows for the definition of strategies tailored to individual needs, promoting not only pain relief but also functional recovery and the prevention of recurrence.
David Brandão | Osteopath and Physiotherapist
Specialised in Clinical Psychoneuroimmunology
Physiotherapist Card: 3652 | Order of Physiotherapists // Osteopath Card: C-0031697 | ACSS
Integrativa | Health and well-being as a lifestyle