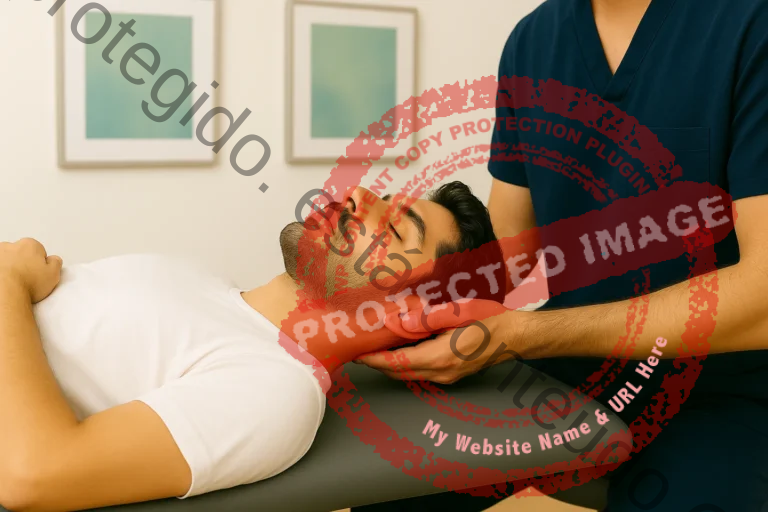
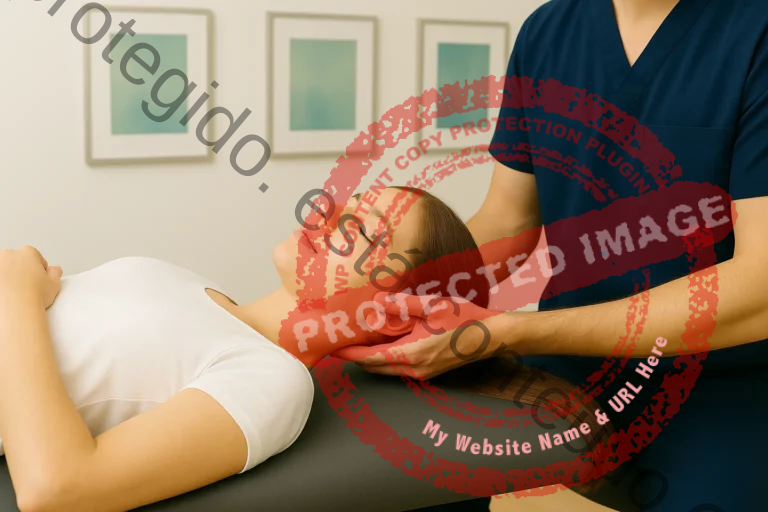
Bruxism is a multifactorial condition characterised by the involuntary grinding or clenching of teeth, frequently associated with factors such as stress, emotional strain and constant worries. Often, the individual is not fully aware of this behaviour, which can be interpreted as a physical response to stress chronic, functioning as an adaptation mechanism to deal with situations of emotional pressure. When not addressed properly, bruxism can have repercussions on oral health and general well-being, potentially leading to musculoskeletal system complications, such as orofacial pain, headaches, and temporomandibular joint (TMJ) dysfunction.
Understanding the underlying causes of bruxism and its effects on the musculoskeletal system is fundamental for an effective clinical approach. Collaboration between different specialties, such as Osteopathy, Physiotherapy, and Clinical Psychoneuroimmunology, allows for a more global approach that considers not only the physical symptoms but also the emotional factors that may contribute to their manifestation.
Bruxism as a response to stress
bruxism is often an involuntary response to stress, with the jaw muscles contracting excessively, generally during sleep. This repetitive contraction generates constant pressure on the TMJ, resulting in muscle tension. Continuous overload can trigger inflammation, causing pain and contributing to chronic headaches, such as tension headaches or migraines.
The relationship between the trigeminal nerve and bruxism
The trigeminal nerve, a major sensory nerve of the face, plays an important role in both pain perception and the regulation of sensory functions of the craniofacial region, including the jaw, teeth, chewing muscles, and the temporomandibular joint (TMJ). In addition to conducting pain signals, the trigeminal nerve also innervates the chewing muscles, such as the masseter, temporalis, and pterygoids, which are responsible for jaw movement.
In the context of bruxism, the muscle tension resulting from the overloading of these muscles can lead to hyperstimulation of the trigeminal nerve. This hyperstimulation creates a feedback mechanism that intensifies pain and muscle tension. As the stress As emotional tension increases, trigeminal nerve activity intensifies, transmitting more severe pain signals. This dynamic contributes to muscle overload and worsening tension, as the nerve also participates in the modulation of muscle contraction. The nerve transmits not only pain signals but also signals that induce involuntary muscle contractions.
Consequently, as the masticatory muscles contract due to stress and bruxism, the trigeminal nerve sends stimuli that perpetuate tension and pain, creating a vicious cycle of pain and muscle hypertonia. This continuous cycle of trigeminal nerve activation and muscle tension can further aggravate bruxism and its associated symptoms, making the condition more difficult to control without an adequate therapeutic approach.
Implications of bruxism on the musculoskeletal system
Overactivity of the jaw muscles, such as the masseter, temporalis, and pterygoids, can lead to significant muscle strain, causing orofacial pain, muscle tension, and chronic headaches. Accumulated tension in the chewing muscles can radiate to areas like the forehead, jaw, temples, and neck, contributing to the development of tension headaches or even migraines.
The TMJ, functionally linked to the skull and cervical spine, can also be affected. The anatomical relationship between these structures helps explain the frequent association between bruxism, headaches, and neck tension. Continuous overloading of the musculature can cause inflammation, worsening the pain and resulting in limitations in jaw mobility and sleep disturbances.
Over time, repeated contraction of the masticatory muscles can cause significant strain on the temporomandibular joint (TMJ), skull, and upper cervical spine, leading to symptoms such as:
Persistent orofacial pain
Tension or migraine headaches
Neck stiffness and pain
Limited mandibular mobility
Changes in cervico-cranial postural pattern
The ATM is integrated with the skull and cervical spine, meaning dysfunctions in this region can manifest as referred pain in the head, neck or shoulder blade area, making clinical assessment more complex.
Clinical evaluation of bruxism
The clinical assessment of bruxism must be comprehensive and personalised. In addition to observing dental wear or hypertrophy of the masticatory muscles, it is essential to analyse:
The mobility and positioning of the TMJ
The tone and coordination of the masticatory muscles
The relationship between the skull, jaw, and cervical spine
Global breathing and tension patterns
Emotional and behavioural factors associated with stress
It is important to highlight that not all cases of bruxism present evident structural dysfunction of the TMJ, which reinforces the importance of a detailed functional evaluation and not just a local one. The identification and treatment of dysfunctions associated with this condition require a thorough and attentive clinical eye.
Osteopathic approach to bruxism
Osteopathy focuses on the biomechanical component of bruxism, with the aim of improving the functional balance of the TMJ and associated structures. Osteopathic intervention acts on the mechanical, neurological, and functional mechanisms involved, in order to:
Reduce excessive tone in the chewing muscles, such as the masseter, temporalis and pterygoid muscles
Improve TMJ mobility
Normalise the relationship between the skull, mandible and cervical spine
Influence the autonomic nervous system
Reduce compensation patterns and muscle overload
Cranial Osteopathy can be particularly relevant when working with cranial structures and the neurovegetative pathways associated with the trigeminal nerve, promoting more effective neuromuscular regulation and helping to reduce pain-related central sensitization.
Using techniques such as joint mobilisations, myofascial release and specific TMJ exercises, Osteopathy can help reduce tension in the jaw, skull and neck muscles, improve local circulation and promote joint mobility. Muscles such as the masseter, temporalis and pterygoids, directly involved in chewing, are often affected in bruxism, as are neck muscles like the upper trapezius and sternocleidomastoid, which can be related to tension headaches.
Osteopathy can also act on cranial tensions, the meningeal membranes and the functional relationship between the skull, the temporomandibular joint (TMJ) and the cervical spine. In cases of headaches associated with bruxism, osteopathic intervention can focus on relieving muscular tension in the head and neck region, promoting improvement in muscular coordination and joint mobility.
The combination of Osteopathy with Physiotherapy can contribute to muscle rehabilitation, helping to reduce muscular overload and improve TMJ function. This integrated approach can be useful in reducing tension, restoring muscular and joint function, as well as aiding in the relief of tension headaches associated with bruxism.
The Osteopathy consultation should be tailored to the specific needs of each patient, considering the intensity and frequency of headaches, trigger factors, and the general state of health. The aim is not only to alleviate immediate symptoms but also to promote long-term improvement in neuromuscular balance, contributing to the patient's well-being.
An integrated and multidisciplinary approach to bruxism
Bruxism is a multifactorial condition that can benefit from an integrated approach, involving collaboration between Osteopathy, Physiotherapy, Psychology, and Dentistry. While Osteopathy and Physiotherapy address mechanical and neuromuscular dysfunctions, Psychology can help manage the emotional factors associated with it. stress, and Dentistry intervenes when necessary for dental protection or occlusal correction. This integrated approach facilitates the understanding of the underlying causes of bruxism and allows for the development of a personalised strategy for each patient, focusing not only on symptom reduction but also on improving neuromuscular function and balance.
Understanding bruxism from an integrative perspective
The approach to bruxism should be comprehensive, given its multifactorial nature, considering not only the physical aspects but also the associated emotional and neuromuscular factors. Beyond the temporomandibular joint and the masticatory muscles, a detailed clinical evaluation is essential to understand the origin of the problem and tailor the intervention to each patient's individual needs.
At Integrative Osteopathy, the fact that our Osteopaths are also specialist Physiotherapists allows for a more comprehensive approach, especially in multifactorial conditions such as bruxism. In an Integrative Osteopathy consultation, we integrate the principles of Clinical Psychoneuroimmunology, an area of knowledge that studies the interaction between the nervous, endocrine, and immune systems. Psychoneuroimmunology also investigates how emotional, behavioural, and environmental factors influence health and the body's adaptive capacity. Osteopathy is complemented by Clinical Psychoneuroimmunology, which educates on lifestyle, sleep hygiene, and relaxation strategies. In this context, the Osteopath may include recommendations for relaxation techniques, such as breathing exercises, to help reduce muscle tension and improve the patient's general well-being.
This integrative approach aims not only to alleviate immediate symptoms but also to promote effective bruxism management and improve the patient's quality of life, with a focus on long-term prevention and adaptation.
At Integrativa, specialised consultations for the TMJ and orofacial pain are part of a global clinical assessment, where the body is analysed in an integrated way, through physiotherapy and osteopathy, considering the interactions between the musculoskeletal (Structural Osteopathy), visceral (Visceral Osteopathy) and cranial (Cranial Osteopathy) systems. A complete and personalised clinical assessment allows for each situation to be framed in detail and for strategies tailored to individual needs to be defined.
The assessment consultation with a specialised Physiotherapist – Osteopath allows for a careful and individualized understanding of how this integrative approach can be beneficial for your case.
David Brandão | Osteopath and Physiotherapist
Specialising in Cranial Osteopathy for TMJ, Orofacial Pain and Headaches
Physiotherapist Card: 3652 | Order of Physiotherapists // Osteopath Card: C-0031697 | ACSS
Integrativa | Health and well-being as a lifestyle