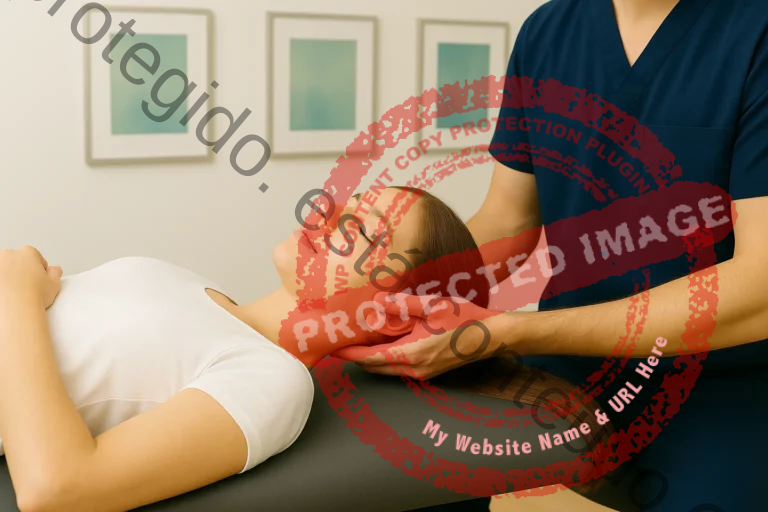
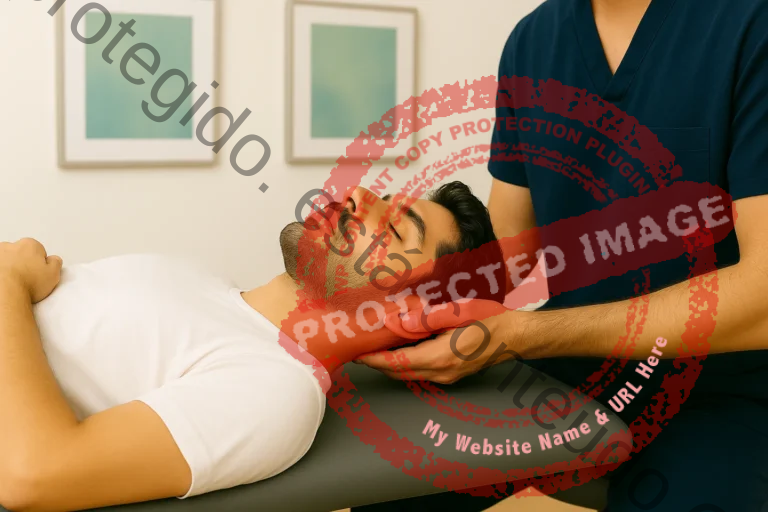
Neck pain is a common complaint in the adult population. Although it is often associated with alterations in the cervical spine, its origin is not always exclusively in this region. In certain clinical conditions, neck pain may be related to alterations in the trigeminal nerve, often associated with dysfunction of the temporomandibular joint (TMJ), which may influence the manifestation or maintenance of symptoms.
This relationship may be more relevant in situations of persistent or recurrent pain, in which approaches centred on the cervical spine alone have limited effectiveness.
The trigeminal nerve and its relationship with neck pain
The trigeminal nerve is the fifth cranial nerve and plays a central role in the sensitivity of the face, oral cavity and part of the cranial region. In addition to its facial sensory function, it establishes functional links with the upper cervical segments, namely C1 and C2, through the trigeminal-cervical complex. This area of neurological convergence allows the integration of afferents from the craniofacial and cervical regions.
This anatomical and functional interconnection may explain why alterations in the trigeminal system, associated with the temporomandibular joint (TMJ), can manifest in the form of neck pain, even in the absence of relevant structural alterations in the cervical spine, a phenomenon described in the literature in the context of the trigeminal-cervical complex (Castien, 2019).
Mechanisms involved in trigeminal-related neck pain
When the trigeminal nerve is sensitised, for example in the context of temporomandibular joint (TMJ) dysfunction, bruxism, persistent tension in the muscles of mastication, sinusitis or interventions in the craniofacial region, this sensitisation can have repercussions in the upper cervical segments. In these cases, the pain is perceived in the neck, even though its functional origin is related to cranial or orofacial structures.
The process can also occur in the opposite direction. Cervical alterations, such as sustained muscle tension, mobility restrictions or inadequate postural patterns, can influence the upper cervical levels, which share neural pathways with the trigeminal nerve. This bidirectional mechanism can contribute to a cycle of perpetuating pain, making it difficult to resolve when only one of the regions is considered.
From a clinical point of view, this reality reinforces the importance of not interpreting neck pain exclusively as a local problem.
Clinical signs that may indicate trigeminal or temporomandibular joint involvement
Some signs may indicate the involvement of the trigeminal nerve or the TMJ in neck pain:
- Neck pain associated with irradiation to the head, face or jaw
- Headaches occurring in association with neck pain
- Persistent feeling of neck stiffness, particularly in contexts of stress or bruxism
- Pain in the occipital region that may extend anteriorly
The presence of these signs justifies a more comprehensive clinical assessment that includes not only the cervical spine, but also the cranial region and the temporomandibular joint (TMJ).
Osteopathic approach to trigeminal neck pain
When neck pain involves the trigeminal nerve, interventions centred exclusively on the neck may have limited or transient effects. In such cases, it is important to integrate an assessment of the cranial structures, the temporomandibular joint (TMJ) and its functional relationship with the cervical spine.
When neck pain is associated with the trigeminal nerve, Cranial Osteopathy emerges as a useful approach, as it does not limit itself to treating only the neck but also considers the skull and the temporomandibular joint (TMJ). Osteopathy aims to promote functional balance between these areas, taking into account the interconnection between the trigeminal and cervical systems.
Treatment includes gentle manual techniques that aim to improve the mobility of the cranial sutures and relieve tension in the facial and neck muscles. Joint mobilisations can be applied to help improve TMJ movement, while myofascial release seeks to reduce tension in the jaw and neck muscles, such as the trapezius and sternocleidomastoid, which often contribute to pain.
Furthermore, Osteopathy also acts on the autonomic nervous system, helping to improve neuromuscular balance, which can reduce pain and help prevent future episodes. Mobilisation techniques for the membranes of the skull can also be applied, as well as improving blood and lymphatic circulation in the area to relieve tension and enhance the overall health of the affected region.
With this approach, Osteopathy aims not only to relieve neck pain but also to improve TMJ function and the relationship between the trigeminal and cervical systems, contributing to more long-lasting relief.
Understanding neck pain from an integrated perspective
Persistent neck pain does not always originate exclusively in the cervical spine. In many cases, it results from complex interactions between the cervical spine, the TMJ and the trigeminal nerve, involving a series of muscular, postural and neurological factors.
Osteopathy can be useful for relieving muscle tension, restoring mobility to the cervical spine and promoting balance in the nervous system, which can be essential for managing neck pain and improving function.
An individualised assessment is important, considering not only the musculoskeletal structures but also the interactions between the skull, TMJ and cervical spine, using Cranial Osteopathy for a more complete and effective approach.
At Integrativa, specialised consultations for the TMJ and orofacial pain are part of a global clinical evaluation, where the body is analysed in an integrative manner through Physiotherapy and Osteopathy, considering the interactions between the musculoskeletal (Structural Osteopathy), visceral (Visceral Osteopathy), and cranial (Cranial Osteopathy) systems. A comprehensive and personalised clinical evaluation allows each situation to be framed in detail and for strategies tailored to individual needs to be defined.
The assessment consultation with a specialised Physiotherapist – Osteopath allows for a careful and individualized understanding of how this integrative approach can be beneficial for your case.
David Brandão | Osteopath and Physiotherapist
Specialising in Cranial Osteopathy for TMJ, Orofacial Pain and Headaches
Physiotherapist Card: 3652 | Order of Physiotherapists // Osteopath Card: C-0031697 | ACSS
Reference articles
- Castien, R. F., & De Hertogh, W. (2019). A neuroscience perspective of physical treatment of headache and neck pain. Frontiers in Neurology, 10, 276. https://doi.org/10.3389/fneur.2019.00276
- Bogduk, N. (2003). The anatomy and pathophysiology of neck pain. Physical Medicine and Rehabilitation Clinics of North America, 14(3), 455–472. https://doi.org/10.1016/S1047-9651(03)00041-1
- Bartsch, T., & Goadsby, P. J. (2003). The trigeminocervical complex and migraine: Current concepts and synthesis. Current Pain and Headache Reports, 7(5), 371–376. https://doi.org/10.1007/s11916-003-0032-4
- Biondi, D. M. (2005). Cervicogenic headache: A review of diagnostic and treatment strategies. The Journal of the American Osteopathic Association, 105(4 Suppl 2), 16S-22S.
- Fernández-de-Las-Peñas, C., & Cuadrado, M. L. (2014). Physical therapy for headaches. Cephalalgia, 34(9), 748-756. https://doi.org/10.1177/0333102414530526
Integrativa | Health and well-being as a lifestyle