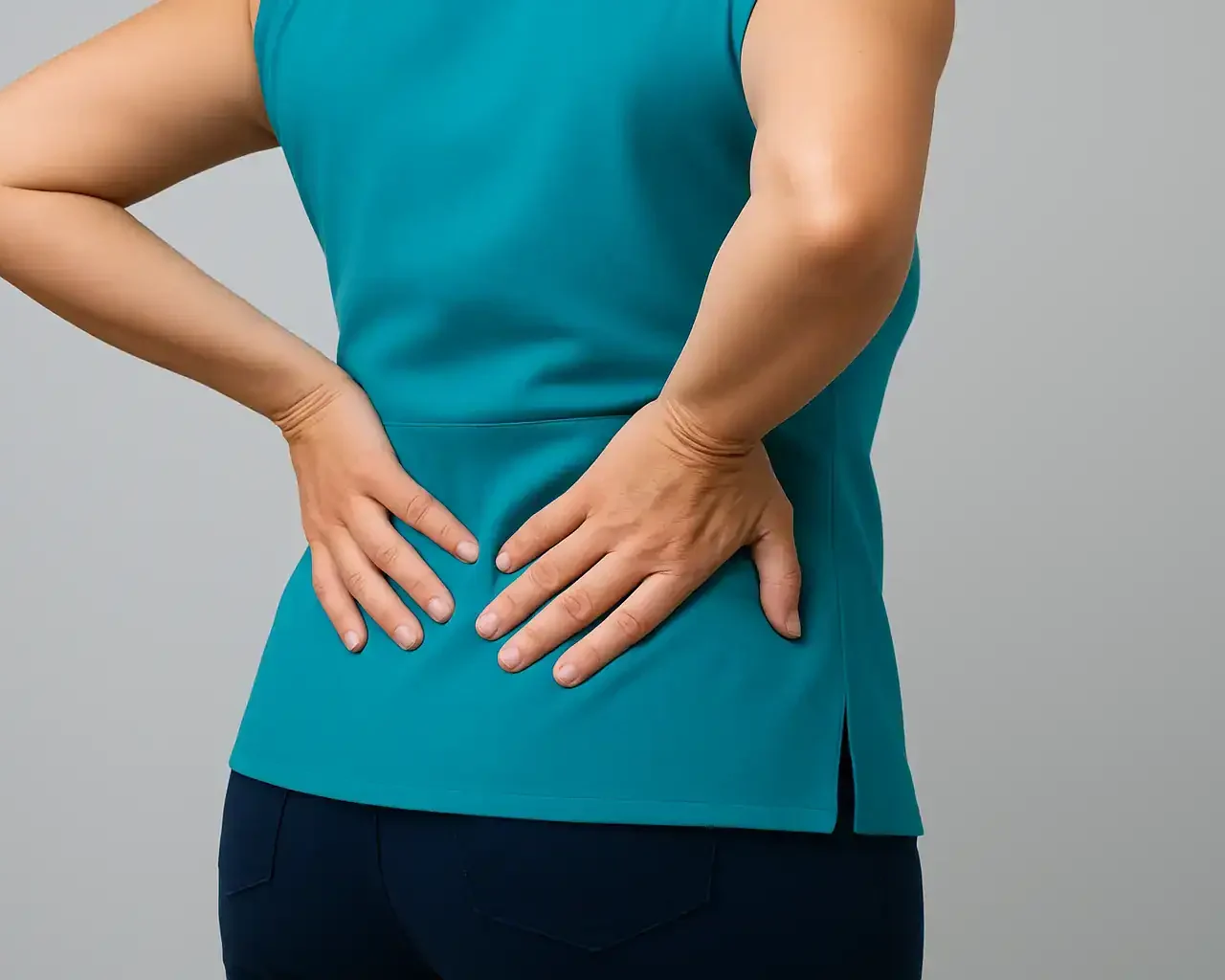
Lower back pain is one of the most common musculoskeletal complaints and a significant cause of functional limitation. Traditionally, its clinical approach has focused predominantly on a biomechanical perspective, concentrating on the spine and adjacent muscular tissues. However, scientific research has increasingly demonstrated that, in some contexts, lower back pain can involve broader functional mechanisms.
Among these mechanisms, the interactions between the gut, the autonomic nervous system and the immune system stand out, particularly in situations of persistent or recurrent pain. It is within this framework that Visceral Osteopathy integrates as a complementary clinical approach, incorporating these relationships into therapeutic reasoning.
The gut as a modulator of musculoskeletal pain
Beyond its role in digestion and nutrient absorption, the gut actively participates in immune and neurovegetative regulation. The intestinal lining acts as a selective barrier, controlling the passage of substances from the intestinal lumen into the systemic circulation and contributing to the maintenance of the body's internal balance.
In certain circumstances, this barrier can present alterations in its permeability, a phenomenon often referred to as increased intestinal permeability. When this occurs, bacterial components, such as lipopolysaccharides (LPS), can cross the mucosa and stimulate the innate immune system. This process has been associated with a state of low-grade systemic inflammation.
When these mechanisms persist over time, systemic repercussions can arise with an impact on pain modulation processes. In this context, understanding lower back pain can benefit from the integration of the gut–brain–musculoskeletal axis, recognising that concomitant changes in these systems can influence how pain is perceived and maintained.
Low-grade inflammation and persistent lower back pain
Low-grade systemic inflammation is characterised by persistently elevated levels of pro-inflammatory mediators, such as interleukin-6 (IL-6), tumour necrosis factor alpha (TNF-α), and interleukin-1 beta (IL-1β). This type of inflammation has been associated, in several studies, with alterations in peripheral and central sensitisation mechanisms.
In some individuals, these processes can contribute to the persistence of lower back pain, even when no relevant structural changes are identified in the spine. In these situations, the pain may reflect not only a local mechanical response but also alterations in the body's regulatory systems.
Referred visceral pain and somato-visceral convergence
Beyond inflammatory mechanisms, the organisation and interpretation of sensory information by the nervous system play a decisive role in the experience of pain. Pain of visceral origin is not always perceived at the site of the organ involved. Visceral and somatic nerve afferents frequently converge in the same segments of the spinal cord, a phenomenon known as somato-visceral convergence.
This neuroanatomical organisation can lead to an inaccurate perception of the origin of nociceptive stimuli, giving rise to what is termed referred visceral pain. Thus, visceral functional alterations, including gastrointestinal tract dysfunctions, can, in some cases, manifest as pain in distant musculo-skeletal regions, such as the lumbar, dorsal, or pelvic area.
This mechanism helps to understand why, in certain clinical situations, interventions focused exclusively on the musculoskeletal structure may not result in sustained pain relief. When the visceral or neurovegetative component is not considered, some contributing factors may remain active, favouring the persistence or recurrence of symptoms.
Integrating the concept of referred visceral pain into the assessment process allows for a broader understanding of low back pain and other complex musculoskeletal complaints, supporting clinical decisions that are better aligned with the overall functioning of the organism.
The vagus nerve in inflammatory and pain regulation
The vagus nerve plays a central role in communication between the central nervous system and visceral organs. Through the cholinergic anti-inflammatory reflex, it participates in the modulation of the immune response and the regulation of systemic inflammation.
Scientific evidence suggests that adequate vagal tone is associated with a greater capacity for self-regulation, reduced inflammatory reactivity, and better adaptation to stress Physiological. Alterations in this pathway may be associated, in some contexts, with the maintenance of persistent inflammation and pain.
Visceral Osteopathy: clinical framework
Visceral Osteopathy is based on the manual assessment and intervention of the mobility, tensions, and functional relationships of internal organs with the musculoskeletal system and the autonomic nervous system.
In the context of lower back pain, osteopathic intervention may include:
- Assessment of visceral and fascial mobility
- Identification of restrictions with potential functional impact
- Support for neurovegetative regulation
- Integration of visceral function into global clinical reasoning
This approach does not replace other therapeutic interventions, and can be integrated complementarily in specific clinical contexts, especially when there are signs consistent with visceral involvement or autonomic dysfunction.
The integrative approach to low back pain
At Integrativa, Visceral Osteopathy consultations are part of a global clinical approach, where we assess the body in an integrative way, considering the interactions between the musculoskeletal (Structural Osteopathy), visceral (Visceral Osteopathy), and cranial (Cranial Osteopathy) systems.
Book an assessment with an Osteopath specialising in Visceral Osteopathy and discover, in a careful and personalised way, how this integrative approach can help with your specific case.
David Brandão | Osteopath and Physiotherapist
Specialised in Visceral Osteopathy and Clinical Psychoneuroimmunology
Physiotherapist Card: 3652 | Order of Physiotherapists // Osteopath Card: C-0031697 | ACSS
Reference articles
- de Punder, K., & Pruimboom, L. (2015). Stress induces endotoxemia and low-grade inflammation by increasing barrier permeability. Frontiers in Immunology, 6, 223. https://doi.org/10.3389/fimmu.2015.00223
- Pavlov, V. A., & Tracey, K. J. (2012). The vagus nerve and the inflammatory reflex-linking immunity and metabolism. Nature Reviews Endocrinology, 8(12), 743-754. https://doi.org/10.1038/nrendo.2012.189
- Vermeulen, W., De Man, J. G., Pelckmans, P. A., & De Winter, B. Y. (2014). Neuroanatomy of lower gastrointestinal pain disorders. World Journal of Gastroenterology, 20(4), 1005-1020. https://doi.org/10.3748/wjg.v20.i4.1005
- Di Vincenzo, F., et al. (2023). Gut microbiota, intestinal permeability, and systemic inflammation: Current evidence and future therapeutic interventions. Frontiers in Immunology, 14, 10954893. https://doi.org/10.3389/fimmu.2023.10954893
- Liu, F. J., et al. (2024). Non-invasive vagus nerve stimulation in anti-inflammatory therapy: Mechanisms and clinical applications. Frontiers in Neuroscience, 18, 1490300. https://doi.org/10.3389/fnins.2024.1490300
- Dmytriv, T. R., et al. (2024). Intestinal barrier permeability: The influence of gut microbiota, diet and exercise. Frontiers in Physiology, 15, 1380713. https://doi.org/10.3389/fphys.2024.1380713
- Macura, B., et al. (2024). Intestinal permeability disturbances: Causes, diseases and therapeutic approaches. Clinical and Experimental Medicine. https://doi.org/10.1007/s10238-024-01496-9
- Siopi, E., et al. (2023). Gut microbiota changes require vagus nerve integrity to modulate inflammation and the vagal afferent pathway. Molecular Psychiatry, 28(12), 5501-5513. https://doi.org/10.1038/s41380-023-02071-6
Integrativa | Health and well-being as a lifestyle