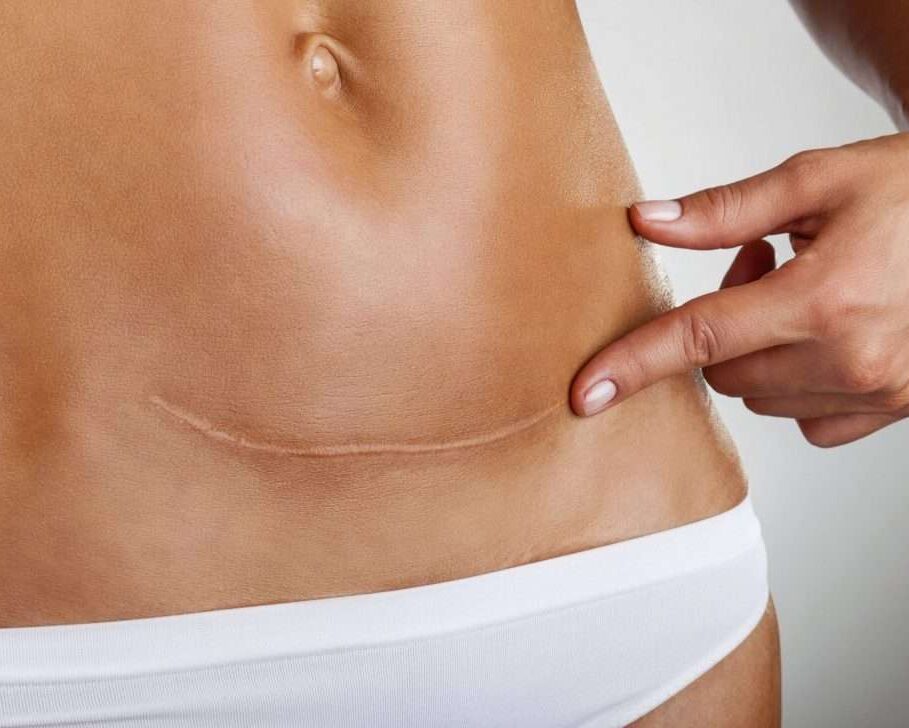
Scars result from the physiological process of tissue repair that occurs after injury, surgery, or trauma. This process involves an organised sequence of cellular events, including inflammation, proliferation, and remodelling, with the aim of re-establishing the structural continuity of the tissues. Despite being essential, scar tissue has different biomechanical and histological properties from the original tissue.
Scars can present with different morphological characteristics, such as atrophic, hypertrophic, or keloid scars, depending on factors like the type of injury, the inflammatory response, and local healing conditions. Beyond the skin, the scarring process can involve deeper planes, including subcutaneous tissue, fascia, muscle, and neurovascular structures.
Besides their visible appearance, scars can be associated with changes in local tissue mobility and sensitivity. Their clinical relevance is therefore not limited to aesthetics, and they can have functional implications in certain contexts.
Caesarean section scars: clinical and functional framework
Scars resulting from a Caesarean section are an example of a deep surgical scar, involving multiple anatomical planes of the abdominopelvic region. The incision passes through the skin, subcutaneous tissue, fascia, muscle, uterus and placenta, leading to a complex healing process.
Although the caesarean section is a widely used procedure and, in many cases, necessary for maternal-fetal safety, the resulting scar can be associated, in some individuals, with local functional changes, such as decreased tissue mobility, altered sensation, or discomfort in the scar region.
The experience associated with surgery and the postpartum period can influence how the scar is perceived, making it important that the clinical approach considers the woman's physiological and emotional context.
From a functional perspective, some people with a caesarean scar report local discomfort, a pulling sensation, or changes in the abdominopelvic region. Complaints may also arise in adjacent areas, such as the lower back or pelvis. These manifestations should be analysed individually, considering postural factors, movement patterns, and adaptation mechanisms over time.
In certain cases, changes in local sensitivity or the behaviour of soft tissues can be observed, as well as signs consistent with alterations in lymphatic drainage, such as local oedema. These situations are not universal and require a case-by-case assessment.
The role of the Physiotherapist in the assessment and monitoring of scars
Given that scars can lead to local changes in mobility, sensation, or function, clinical evaluation by specifically trained healthcare professionals may be relevant in certain contexts. In Physiotherapy, observation, palpation, and functional assessment allow for the characterisation of the scar and an understanding of its relationship with movement and overall body function.
The assessment in Physiotherapy of a scar includes the analysis of its morphological characteristics, tissue quality, superficial and deep mobility, sensitivity and its relationship with movement patterns, posture and breathing. This integrated reading allows for the identification of how the scar may be interfering with the body's functional organisation.
In the case of surgical scars, such as those resulting from a caesarean section, the assessment extends to the abdominal wall, the lumbopelvic region, and strategies for stabilisation and motor control, considering the impact of the scar on movement patterns and functional adaptation over time.
Based on this assessment, the Physiotherapist can identify tissue restrictions, changes in elasticity, areas of hypersensitivity, or mobility deficits that may interfere with function. The intervention is individually tailored and may include therapeutic education, tissue mobilisation techniques, sensory re-education, and progressive integration of the scar into functional movement, always respecting the healing phase and individual tolerance.
A central aspect of the physiotherapist's role is educating the patient in scar self-care. Appropriate guidance allows for an understanding of the healing process, recognition of relevant signs and active participation in recovery, respecting the biological adaptation times of the tissues.
The therapeutic approach of Physiotherapy to scars is not solely focused on local improvement, but can also consider their integration into the body's overall function. In this way, the Physiotherapist helps to support comfort, functionality, and progressive adaptation to daily demands, safely and tailored to individual needs.
Understanding scars from a functional perspective
Scars are not just visible marks on the skin. They represent structural adaptations of the organism after tissue damage and, in some cases, can be associated with local functional changes that warrant clinical monitoring.
Attention to scars, particularly those resulting from surgeries such as caesarean sections, allows for their assessment to be integrated into the overall context of the individual's functionality. Proper assessment and monitoring contribute to better integration of the scar into the body's functioning, supporting comfort, functionality, and the recovery process.
When there are persistent symptoms, changes in sensation, or functional limitations associated with a scar, assessment by a Physiotherapist trained in scar assessment and treatment can help to understand the clinical picture and define strategies tailored to individual needs.
David Brandão | Osteopath and Physiotherapist
Physiotherapist Card: 3652 | Order of Physiotherapists // Osteopath Card: C-0031697 | ACSS
Integrativa | Health and well-being as a lifestyle